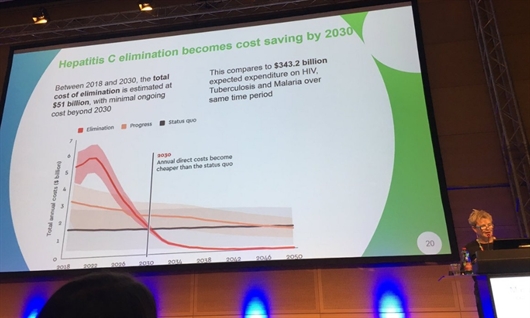
Margaret Hellard of the Burnet Institute presenting their modelling study at The International Liver Congress. Image: @AnnetteGaudino and @TAGTeam_Tweets
Most countries will
struggle to eliminate hepatitis C by 2030 due to lack of investment and
political will, missing an internationally agreed target set by the World
Health Organization, The International Liver Congress in Vienna heard earlier
this month.
“Despite the progress we’ve seen, we’re clearly not going to make
it,” said Gottfried Hirnschall, Director of HIV and Hepatitis at the World
Health Organization (WHO), speaking at a symposium on elimination of viral hepatitis
organised by WHO.
The World Health Assembly agreed ambitious targets for elimination
of viral hepatitis in 2016. Countries pledged to scale up prevention, diagnosis
and treatment so that deaths caused by viral hepatitis would be cut by 65% and
new infections cut by 90%
Although 124 countries now have national plans for viral hepatitis
elimination, 42% of plans have no domestic funding, Mark Bulterys, head of
WHO’s hepatitis team told the symposium.
Furthermore, although 5 million people had been treated with
direct-acting antivirals by the end of 2017, most of these treatments occurred
in ten 'champion countries' which have scaled up treatment quickly, including
Egypt, Brazil and Australia.
Even in higher-income countries, hepatitis C elimination may only
be achieved by a handful of countries by 2030, the Center for Disease Analysis
estimates. Nine countries – Australia, France, Iceland, Italy, Japan, South
Korea, Spain, Switzerland and the United Kingdom – will achieve elimination by
2030 at current rates of diagnosis and treatment.
Modelling by Stanford University for WHO estimates it will cost
$58.8 billion to achieve elimination of viral hepatitis by 2030, slightly
higher than the $51 billion estimate presented by Professor
Margaret Hellard of the Burnet Institute, Melbourne, on the opening
day of the conference.
To speed up progress towards elimination, WHO emphasised the need
for:
- Lower-income countries to take
advantage of voluntary licensing agreements that permit the importation of
low-cost quality-assured direct-acting antivirals.
- Countries to develop national plans
for viral hepatitis elimination and to commit domestic funding to elimination.
- Adoption of simplified treatment and
monitoring protocols – including task shifting to general practitioners, nurses
and community health workers – that will enable larger volumes of people to be
diagnosed and treated.





Connect with infohep on Facebook: Keep up to date with all the latest news and developments.
Follow infohep on Twitter for links to news stories and updates from infohep.org. Follow us at www.twitter.com/infohep.
Follow all the infohep news by subscribing to our RSS feeds.